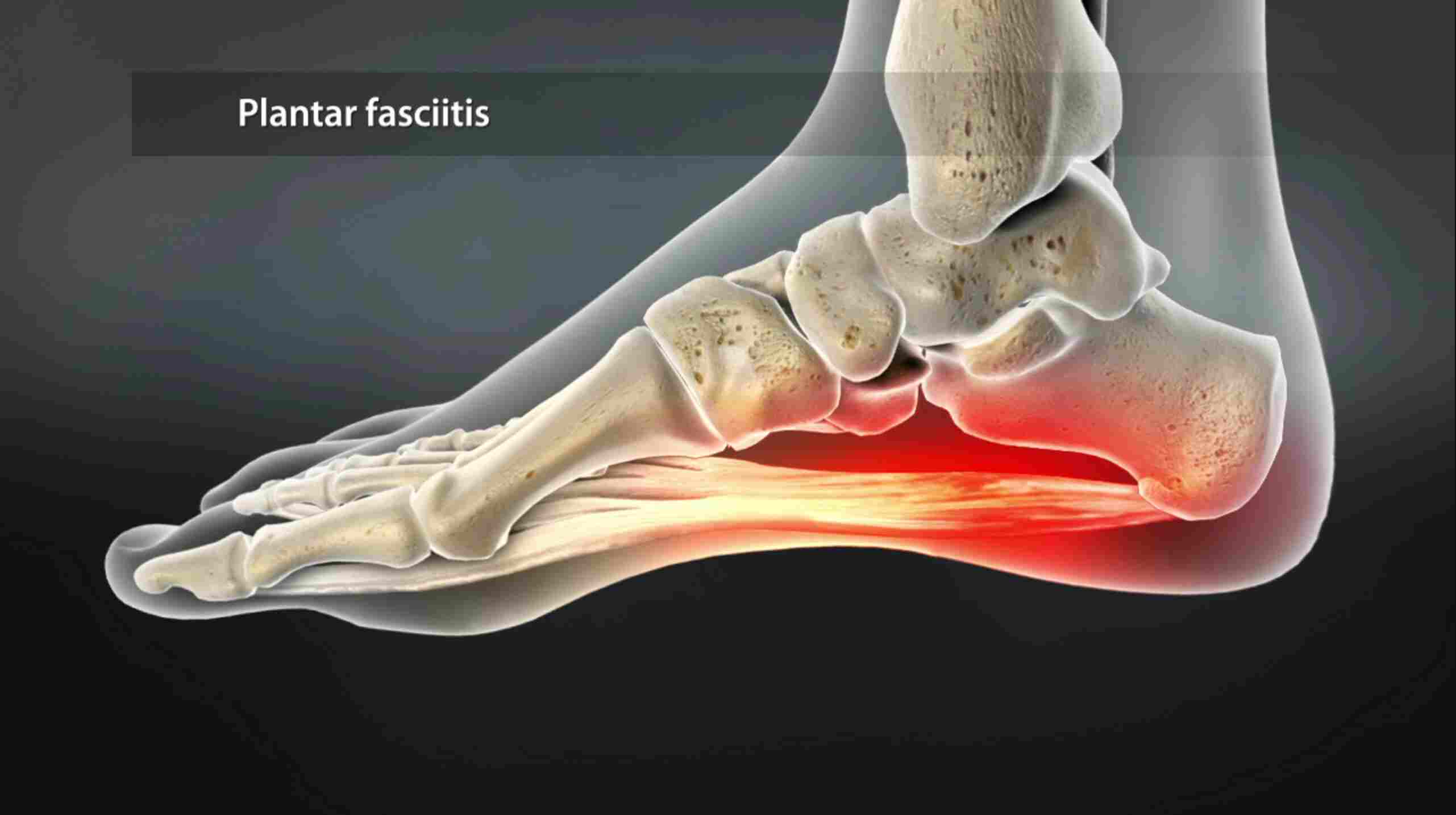
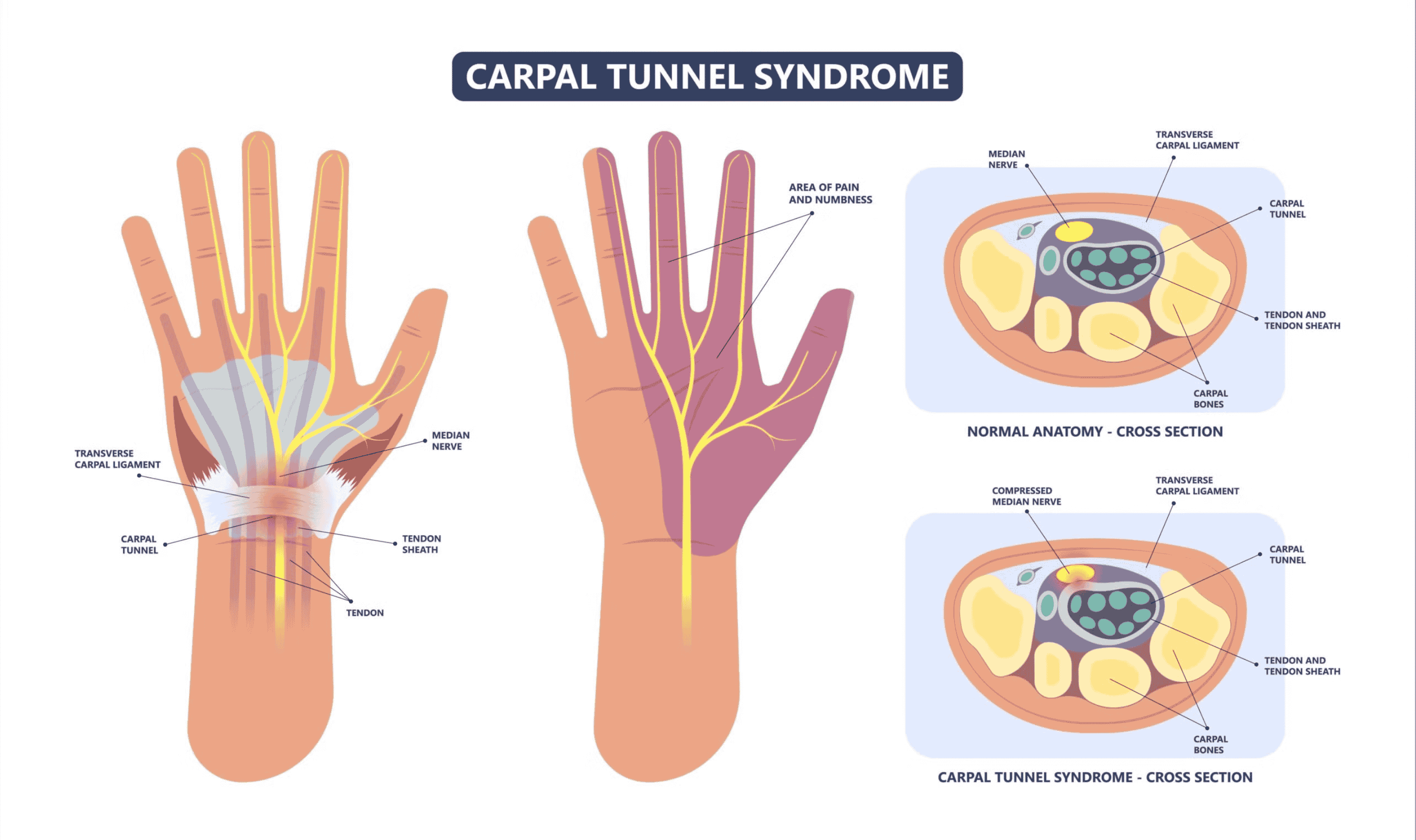
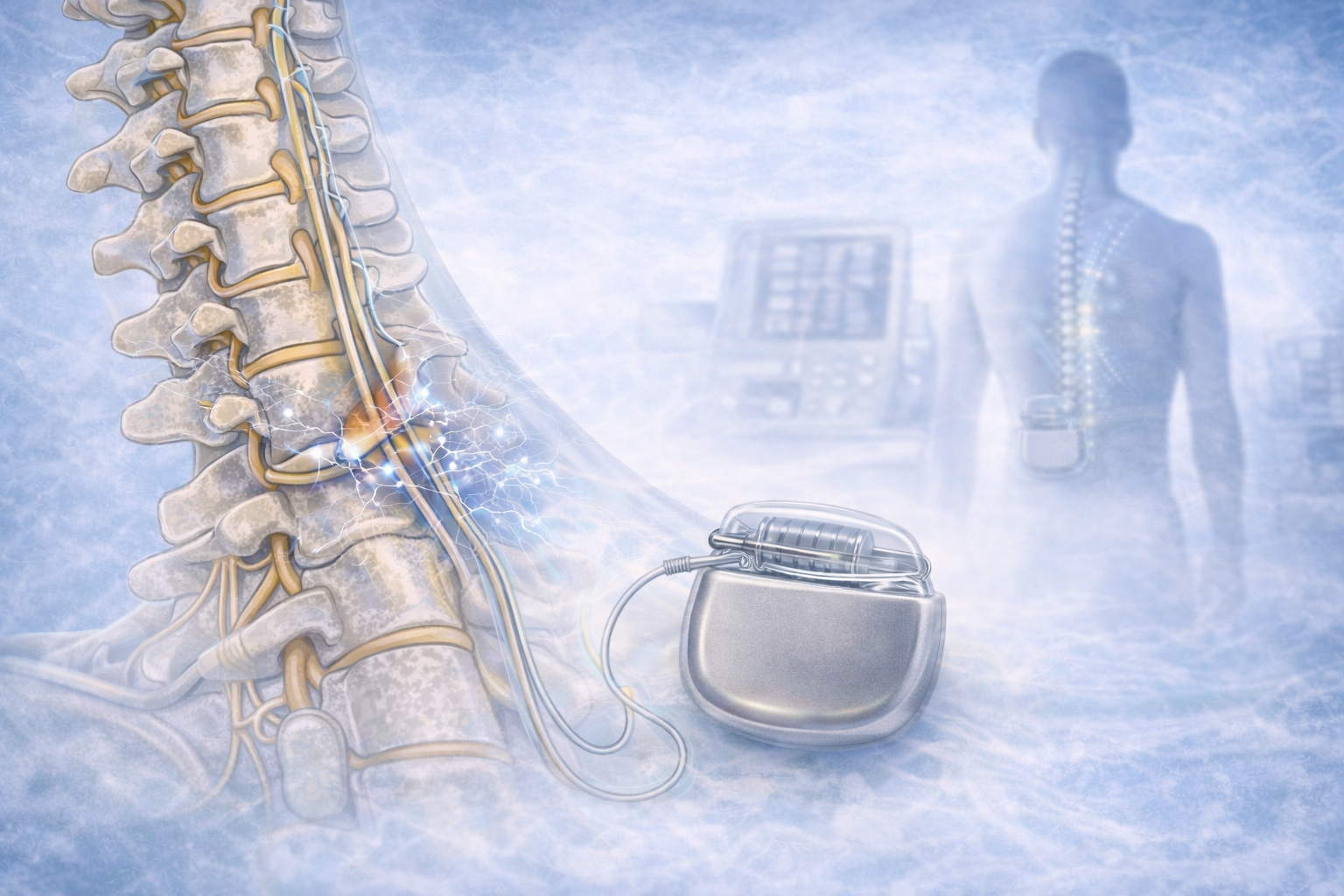
diabetic neuropathy
Diabetic neuropathy is a complication of diabetes that results from damage to the nervous system. It is a progressive disease, and symptoms get worse over time.
Neuropathy happens when high levels of fats or sugar in the blood damage the nerves in the body. It can affect virtually any nerve in the body, with a wide range of symptoms.
Nerves are essential to managing, how the body works. They allow to move, send messages about how things feel, and control automatic functions, such as breathing sweating, urination etc.
There are several types. Some involve the peripheral nerves, while others damage the nerves that supply the internal organs, such as the heart, the bladder, and the gut. In this way, it can affect many body functions.
30-50% of people with diabetes have neuropathy, according to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK).
We explore the different types, effects, and risks of diabetic neuropathy.
Four main types of neuropathy can impact the nervous system, including:
-
Peripheral symmetric neuropathy: This affects the feet and hands. It is the most common form of diabetic neuropathy.
- Autonomic neuropathy: This occurs in the nerves that control involuntary functions of the body, such as digestion, urination, or heart rate.
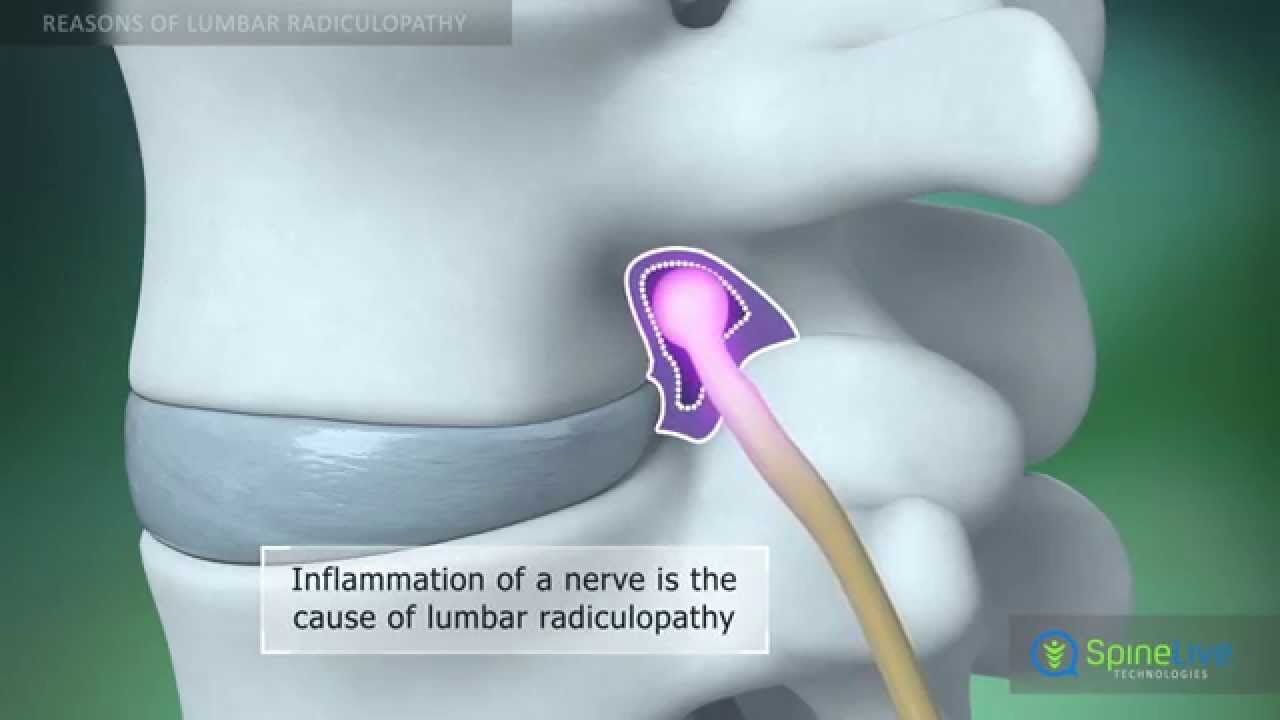
- Thoracic and lumbar root, or proximal, neuropathy: This damages nerves along with a specific distribution in the body, such as the chest wall or legs.
- Mononeuropathies: These can affect any individual nerve.
The symptoms of neuropathy depend on the type and the nerves involved.
The signs and symptoms of diabetic neuropathy usually take several years to appear. Signs and symptoms will depend on which type of neuropathy and nerves it affects.
Peripheral neuropathy
The symptoms of peripheral neuropathy include:
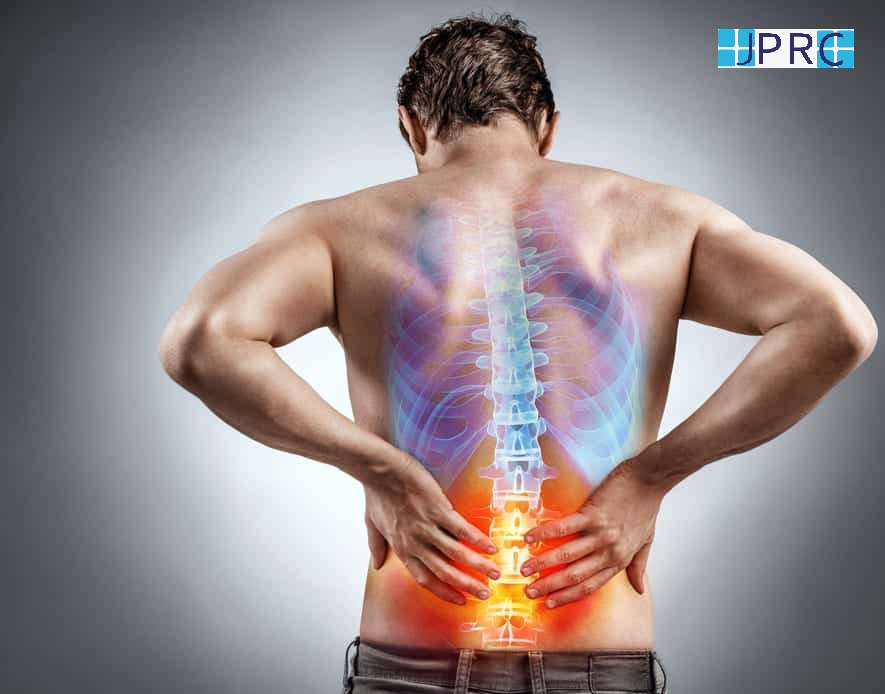
- Numbness, pain, tingling, and burning sensations starting in the toes and fingers then continuing up the legs or arms
- Loss of muscle tone in the hands and feet
- Not being able to feel the heat, cold, or physical injury
- Loss of balance
- Charcot’s joint, in which a joint breaks down because of nerve issues, often in the feet
Peripheral neuropathy that affects the feet can make it difficult for a person to stand and walk. It can increase the risk of falling.
When a person cannot feel heat, cold or injury, this can lead to new problems.
For example, a blister on the foot can become ulcerated because the person did not feel pain in the early stages. As the infection progresses, Gangrene can develop.
Eventually, amputation may be necessary.
Autonomic neuropathy
The effects of autonomic neuropathy include:
- Heartburn and bloating sensation
- Nausea, constipation, restlessness
- Hypoglycemic unawareness, in which a person does not feel the effects of low sugar levels
- Difficulties speaking or swallowing
- Feeling full after eating small amounts of food
- Vomiting several hours after eating
- Orthostatic hypotension or postural hypotension or feeling light-headed and dizzy when standing up
- A faster heart rate than normal
- Sweating, even in cool temperatures or while at rest
- Bladder problems, for example, difficulty emptying the bladder completely when urinating, leading to incontinence
- Sexual dysfunction in men and women
- Dysesthesia, or a distorted sense of touch
- Significant drooping of the face and eyelids
- Muscle contractions and weakness
Other types
There are many types of neuropathy.
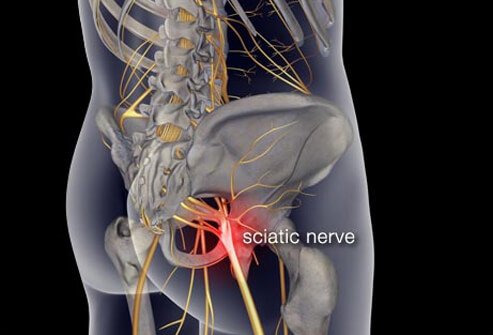
Proximal neuropathy can lead to pain in the lower body, often on one side, and weakness in the legs.
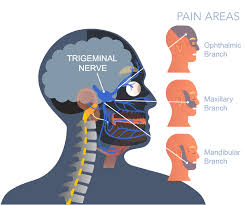
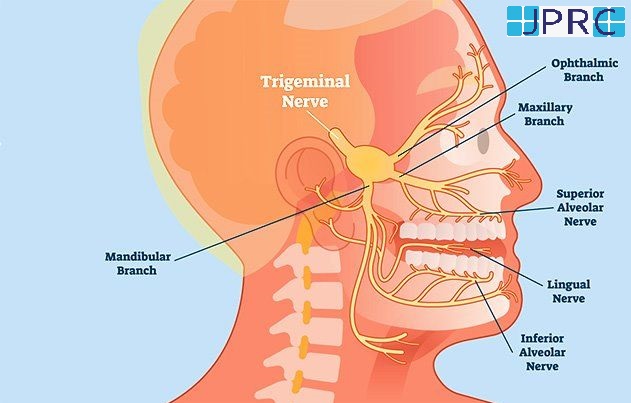
Symptoms of focal neuropathy can vary widely, depending on the nerve affected. Focal neuropathy and cranial neuropathy can both lead to visual disturbances, such as diplopia or double image.
People with diabetic neuropathy often do not realize they have it until the symptoms are more advance
Diagnosis-
A physician will carry out a physical exam and foot exam to check for:
- Ankle reflexes
- Loss of sensation
- Changes in skin texture
- Changes in skin colour
Other tests may include a check of blood pressure and fluctuations in heart rate.
If the doctor suspects diabetic neuropathy, they may run some diagnostic tests, such as:
- An electromyogram (EMG), which records electrical activity in the muscles
- A nerve conduction velocity test (NCV) records the speed at which induced signals pass through the nerves
Treatment
Most types of diabetic neuropathy get worse over time.
The first step for people with any type is to bring blood sugars within a target range agreed with a doctor and manage High BP and cholesterol levels.
Managing glucose levels will minimize the risk of diabetic neuropathy. A key part of the treatment focuses on reducing pain and managing some of the symptoms.
Medicine and different types of therapies can help to control the pain of diabetic neuropathy, alongside other treatments. However, they cannot repair the nerves.
People should also avoid or stop smoking and limit their alcohol intake to a maximum of one drink a day for women and two for men.
Medications
Drugs that can help to manage pain include:
- Anticonvulsant drugs
- Tricyclic Antidepressant
- Opioids and nonopioid pain relief medication
Opioid use can lead to dependency, so doctors should prescribe as low a dose as possible.
A person with diabetic neuropathy might use other types of antidepressants, such as serotonin-norepinephrine inhibitors, to target other painful symptoms of diabetic neuropathy.
Topical lotions, compound creams, and some supplements, such as ALA or topical capsaicin, may also provide relief.
Physical therapy
Physical therapy, used in combination with medications, might help relieve pain and reduce the risk of dependency on opioids.
It may also help alleviate:
- Burning and tingling sensations in the legs and feet
- Muscle cramps
- Muscle weakness
- Sexual dysfunction
Electrical nerve stimulation is a painless type of physical therapy that might help to reduce feelings of stiffness and enhance the healing of foot ulcers.
Gait training involves relearning how to walk. It helps to prevent and stabilize foot complications, such as ulcers and injury. This type of physical re-education is crucial for people using prosthesis after losing limbs if diabetic neuropathy leads to an amputation.
Pain physician or neurologist will ensure that exercises for people with diabetic neuropathy do not hurt the feet, which can be sensitive.
Other therapies include devices that a person can use to keep painful or sensitive extremities from touching the bed or chair.
Pain physician, massage therapist, or osteopath can carry out regular massages or manual therapy to stretch the muscles. Massage can inhibit muscle contractions, Spasms, and Atrophy due to poor blood supply.
Specific exercises, such as Swimming or Aerobics, can help an individual develop and maintain muscle strength and reduce the loss of muscle mass.

















































.jpg)








_Injection_Description_in_Hindi.jpg)













.jpg)







.jpg)




.jpg)
.jpg)
.jpg)






.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)






1.jpg)
1.jpg)
1.jpg)
1.jpg)
1.jpg)
1.jpg)
1.jpg)








2.jpg)
3.jpg)
4.jpg)
1.jpg)
2.jpg)
5.jpg)
6.jpg)

7.jpg)
2.jpg)

8.jpg)

9.jpg)
3.jpg)

10.jpg)

11.jpg)


12.jpg)
4.jpg)